Monday
 by Danielle Ofri
by Danielle Ofri
(Fictional story, published in “2 Bridges Review” pg 86)
Maybe it was simply human nature that no one wanted to be sick on weekends. Or admit to it. Or do something about it. Whatever the reason, Mondays were always the days of reckoning: weekend walls of denial came crashing down, weekend indiscretions faced their due, weekend warriors paid their price in blood. Admissions poured into the hospital. It was as though the map of Brooklyn had been curled up like a cone and all the human wreckage and misery funneled down to the tip where East Memorial Municipal Hospital sat, as it had for the past century since it opened, with its doors flung widely and indiscriminately open.
On Mondays, Graham and his medical team didn’t even wait for the admissions to come up from the emergency room to the 16th floor medical ward—relying on the logistics of East Memorial’s admissions and transportation services was a sure-fire way to get stuck in the hospital all night. Instead, they trolled the ER, picking up the admissions as soon as they were assigned to the medical team. The doctors performed the history, physical, and initial work-up while the patient was still on the gurney, caught in the warren of interconnecting rooms, alleys, and converted broom closets that constituted the East Memorial ER.
The ER had never been formally expanded; it simply usurped various corners of the hospital as it grew. The official titles of the various subdivisions often oversold the spaces they represented: The Triage Area was simply the line of gurneys in the hallway. The Satellite Observation Unit (the SOU) was a mass of stretchers huddled behind a curtain in a dingy open area, fronted at one end by the glass doors that opened to the incoming ambulances and at the other by a cramped desk from which nurses and doctors grabbed the accumulated charts. The Procedure Room was a dead-end alley off of the main observation unit. The Asthma Room was a poorly-lit corner by the elevators, where one beleaguered nurse offered up nebulizers and oxygen to the legions of Brooklyn’s asthmatics. The Emergency Ward—the supposed ICU in the ER—was an airless back-room, accessible by a single doorway. Through this impossibly narrow entranceway, critically ill patients surrounded by a bevy of interns supporting IV bags, oxygen pumps, portable defibrillators, and other accoutrements of the nearly demised would squeeze through. Team spirit was built by the communal exhalation required to overcome laws of physics that would normally prevent a gurney and four interns from wedging through a 36-inch space.
Only the GYN room was a true room, with an actual door that closed and even locked. However, it doubled as the optho room, since the closed doors and lights made it the only location in the entire ER dark enough to perform proper eye exams. Stirrups and slit-lamps competed for space in this tiny acreage of privacy.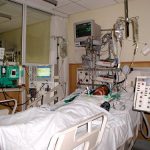
All the walls in the ER were painted some variant of green, based either on a philosophy of the healing properties of the green hues or on a discounted price that the Kings County Municipality had received on a pallet of mismatched green paint during the Depression. Whatever the case, everything everywhere was greenish, though scuff marks, scratches, stains, water marks, mold, graffiti, and time had lent a more mottled appearance to the walls.
As the attending physician supervising his medical team, Graham was really supposed to examine the new patients on the following day. The interns and residents were supposed to do the initial evaluations upon admission, then present the case the next day during formal attending rounds. While that system worked well in the days of yore, it was an impossible anachronism in today’s world of high-volume admissions, decreased length-of-stay, rapid turnaround times, 24/7 diagnostic tests. If there were ten or twelve new admissions, the old orderly system in which the attending pontificated at leisure the next morning with the team was simply an academic pipe dream.
So Graham rolled up his sleeves and divided up the work with the interns and residents to make the process most efficient. He didn’t care much about hierarchies in general, and since he’d finished his residency only five years ago, he didn’t feel particularly high and mighty. Nor did he particularly want to be one of those high and mighty attendings who were so removed from the fray that they forgot how to practice real medicine. Some of Graham’s colleagues donned Brooks Brothers’ suits the minute they surrendered their beepers to the residency program. But Graham still preferred the standard uniform of khaki pants and buttoned-down shirts—no tie of course, and sleeves usually cuffed to the elbow. He was still the same tall, rangy guy with the slight hunch in his shoulders that he’d been as an intern eight years ago. Why should he don fancy clothes or a fancy attitude just because he’d been bumped forward a notch in life? The medicine wasn’t much different, his responsibilities weren’t much different, and frankly his salary wasn’t much different. When he looked in the mirror he saw the same angular face, with the same long, narrow rampart of a nose. When he placed his hands on a patient’s chest he saw the same knobby joints connecting the same spindly, freckled fingers. He was the same guy, doing the same job, just with a couple extra years of experience under his belt and a couple extra crows’ feet stretching out from the corners of his lugubrious gray eyes
Graham looked at his list of patient: “Cherry Milford: 34 y.o. F, skin-popper, fever, leg ulcer.” Graham was combing the ER boards for her name when he felt a booming thunk on the back. “Graham, my man! What’s happening?” It was Sammy Chen, one of his buddies from internship. Sammy once drank an entire bottle of ketchup on a dare when the interns had gone out to a local bar for ‘liver rounds.’ He followed it up with six shots of tequila and never vomited once. Nobody every figured he’d settle on a sedate, intellectual specialty like nephrology. But there he was, running the dialysis unit at their hospital, calculating urine/serum osmolality ratios.
 “Hunting for an admission for my team,” Graham said, elbowing Sammy’s muscled forearm off his shoulder. “What brings a kidney man like you down to the ER?”
“Hunting for an admission for my team,” Graham said, elbowing Sammy’s muscled forearm off his shoulder. “What brings a kidney man like you down to the ER?”
“Moonlighting,” he said, shoving away clump of hair that had tumbled onto his forehead. “I’m thinking of maybe getting a summer place. Gotta save some dough.” Sammy was wearing beat-up basketball sneakers and faded blue scrubs that said, “Property of Grady Hospital: Do Not Remove.” Sammy glanced over to Graham’s list. “Who are you looking for? Maybe I triaged him.”
“Her,” Graham said. “Cherry Milford. 34. Skin-popper.”
Sammy pulled his arms in and folded them over his chest. “A real piece of work,” he said. “I triaged her Milford all right, but Jesus…” Sammy sucked in his breath. “Wait’ll you see.”
“What’s there to see?” Graham said. “She sticks a needle under her skin and now there’s a skin ulcer. Big deal.”
“Hoo-boy, now that’s where you’re misguided,” Sammy said, falling into a boxing stance and throwing jabs at Graham. “Hey, you got to get yourself in shape, man. You’re just skin and bones.” Sammy sunk a mock uppercut to Graham’s jaw. “Anyway, I think your skin-popper’s over in the SOU. It would be my pleasure to edify you with the cutaneous clinical manifestations of skin-popping that Madamoiselle Milford presents with.” He threw one more jab to Graham’s right flank, then set off for the SOU. Graham followed one step behind.
The ER was packed, as was usual on Mondays. The line of gurneys in the triage area stretched along the hallway. In the curtained slots of the examination area, intended for individual patients, there were two gurneys, sometimes three. Family members, clerks, interns, medical students, hospital police, X-ray techs, phlebotomists, admitting staff milled around the patients like shifting fields of meteors, clumping and unclumping, occasionally colliding. The general din was not dissimilar to the subway that rumbled underneath the hospital floorboards every few minutes. Metal instruments clattered, oxygen whooshed, IV machines beeped, blood tubes clinked. Competing shouts crisscrossed the vast room, and astute linguists could detect strands of Spanish, Bengali, Mandarin, Croatian, Cantonese, Tibetan, Arabic, Hindi, Tagalog, Fukienese woven through the predominant language of medical slang. “DKA in 3: start a drip.” “Altered mental status: needs CT/LP.” “Two rule-outs in the corner; first set of enzymes negative.” “4B needs a flat-plate and upright.” “Two units packed cells plus four of FFP, stat.”
Sammy pulled the curtain back on the SOU with a grand gesture. “May I present Mademoiselle Cherry Milford.” Lying there was an emaciated addict whose drug use and street life had aged her a good two decades beyond her chronological age of 34. She lay on the stretcher, her face, lips and posture slack. Her afro stood up in matted clumps from the back of her head, and the white sheets around her were already smudged with dirt. The odor of homelessness was unmistakable. The interns called it toxic sock syndrome, and that was indeed what it was: a pungent blend of curdled sweat, unwashed socks, grime-encrusted feet, unshowered skin.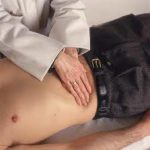
Graham could feel his spirit deflating and he took a half-step back. Sammy raised his eyebrows and gave him an ‘I told you it was a doozy’ look. But it wasn’t the smell so much—though Graham wouldn’t deny that he was squeamish—it was the bare-knuckled pitiableness that got to him. Even though he had treated hundreds of drug addicts and street people during his medical career, the thoroughness with which the world could devitalize a human being always gave him a momentary sock in the gut.
“Ms. Milford here is a little slow on the Aristotelian dialectics,” Sammy said. “I suggest you proceed to the physical exam, Dr. Brenfield. I’m sure the interns will gladly immerse themselves in the myriad minor details of Ms. Milford’s mannered life.” Despite Sammy’s bison-like lack of grace, his words really were true: as the attending, all Graham really needed to know was whether this ulcer needed surgical intervention or whether IV antibiotics would be sufficient. The interns could sort out the rest. Graham bit his lip and tried to ignore the odor as he started the medical interview. Cherry Milford’s answers to Graham’s questions were slurred and incoherent.
“Where’s the ulcer?” Graham asked the patient. Cherry Milford’s index finger, with its dirt-encrusted, ragged nail, wove sluggishly in the air until it landed tentatively in the region of her left thigh.
“Allow me,” Sammy said, grabbing the edge of the sheet. “This is the pièce de résistance.” Sammy slowly pulled the sheet back with exaggerated drama, and Graham grew impatient. He just wanted to eyeball the ulcer, and was expecting the usual quarter-sized wound that most of these skin-poppers inflicted on themselves. But when Sammy folded the sheet all the way back, Graham let out a low whistle. This wasn’t an ulcer; this was a crater.
The entire length and breadth of Cherry Milford’s thigh, from the crease of her groin down to her kneecap, was a scooped-out mass of gravelly pink-white-gray tissue. If Cherry Milford had the strength or inclination to sit up and bend forward, she could probably nestle her entire forearm in there, elbow to fist. Over the years Graham had seen his share of cutaneous injuries from skin popping, but nothing held a candle to this. This was one for the record books, even by East Memorial standards.
“How long have you had this?” he asked, incredulity overtaking jadedness. Even the caustic vinegary smell of it temporarily receded in his consciousness; he just couldn’t believe what he was seeing.
Cherry Milford shrugged in slow motion. “Dunno. Sort of started a while back. I shot up there and it got a little craggy.”
“A little craggy, eh?” Sammy asked. “Didn’t you notice that your entire thigh had practically disappeared?”
“Ms. Milford,” Graham said, trying to focus the patient’s attention. “This is a serious ulcer. We’re going to start IV antibiotics, but we might need the surgeons to clean this out. Do you have allergies to any medications?”
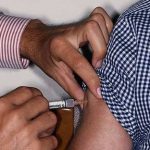 But the particulars of medical treatment were apparently beyond Cherry Milford in her current state. Her eyes were already closing and petite snores gave way to full-throated snorts and snuffles. The anodyne aspects of heroin worked in Ms. Milford’s favor, buffering Sammy Chen’s words as well as the rest of the world from her consciousness.
But the particulars of medical treatment were apparently beyond Cherry Milford in her current state. Her eyes were already closing and petite snores gave way to full-throated snorts and snuffles. The anodyne aspects of heroin worked in Ms. Milford’s favor, buffering Sammy Chen’s words as well as the rest of the world from her consciousness.
“A little craggy, eh?” Sammy repeated, as he and Graham tugged the curtain shut behind them. “Jeez Louise—you could probably store a pair of sneakers and an order of take-out Chinese in that ulcer.” He shook his head in amazement. “You know, there are probably real-estate opportunities here. A little redecorating and it’s a perfect starter apartment. You can rent out anything in this city …”
“I’ll get plastics to take a look at that ulcer,” Graham replied, feeling the need to sound as business-like as possible. “Maybe even ortho—there’ll probably be raw femur sitting in there once all the debris is removed.”
“Like I said,” Sammy said, “the prom-queen.”
“I see you’re in a mighty charitable mood today, Dr. Chen,” Graham said, folding up his list and pressing it into his pocket.
“I’m telling you, man, we had a run of shooters-with-fevers last night. What are these guys mixing up their drugs with—toilet water? With my luck Ms. Milford will shoot her panoply of viruses straight to the kidneys and end up in my fucking dialysis unit. Another $500 dialysis catheter wasted on piss-poor protoplasm.”
“Glad to know you’ve recommitted yourself to the care of the needy and the vulnerable in our city.”
“Fuck off, Brenfield,” Sammy said, giving Graham a quick left-hook to the abdomen. “Gotta cover yourself, brother,” dropping the tenor of his voice. “Someone could pop your spleen if you’re not faster on the draw.”
Graham knew that Sammy wasn’t a complete cynic—there were plenty of doctors who were unabashedly derisive about scumbags, assholes, and gomers who populated the East Memorial ER. Sammy actually cared about doing the right thing for his patients, but he had no patience for what he perceived as self-destructive behavior. Sammy Chen’s dialysis patients could count on superb clinical care, but they had probably learned to get their emotional succor elsewhere.
Graham left Sammy and walked toward the ER nurses’ desk, tugging his fingers through his wiry brown hair. Sheila said that the parts that were graying made him look distinguished. Graham thought they made him look like a guy who was spinning headlong through his thirties with neither a handle on life nor a 401k.
“It’s sexy,” Sheila told him. But all the men in her investment firm with that sexy, graying look were also pocketing millions of dollars in bonuses and sporting double-breasted Italian suits. Graham was still working for East Memorial Municipal Hospital, the same crummy inner-city hospital at which he’d done his residency, and his salary contribution to their marriage was only marginally more than when he was an intern.
He just couldn’t muster the enthusiasm and business interest that was required to build a private practice. He’d applied for gastroenterology fellowships toward the end of residency, but didn’t get into any of the good programs. Sheila would have considered moving out of Manhattan if he’d gotten a spot at Mass General or UCSF, but not for the Kerrville VA in Texas. Staying on at East Memorial was just simpler—Graham knew the routine, and the interns did weekend coverage for his patients. Besides, he wasn’t even sure he wanted to be a gastroenterologist. It seemed that everyone in his residency class marched lock-step toward medical specialties like cardiology and GI, and Graham simply puttered along with the flow toward specialization for lack of a better plan.
But did he really want to spend his life threading tubes into people’s intestines or coronary arteries? Sheila no doubt wanted to be married to a Park Avenue cardiologist, but now she was stuck with a general internist at a city hospital in a non-gentrifying neighborhood in Brooklyn. The staff doctors at East Memorial were city employees like everyone else at the hospital, which meant decent benefits and lousy salaries. How many other women at Sheila’s firm, he wondered, had husbands who possessed union memberships instead of stock options? Sexy indeed.
“Dr. Brenfield,” came a warbly, desperate voice. Graham turned around. It was Hamdi, one of the interns on his team. Everyone called him Hamdi, even the patients, because nobody could swing their mouth around Dr. Hamedian Avarhamian. Hamdi looked perpetually harried, even at 7 a.m. But by late afternoon, as it was now, he seemed on the verge of a nervous breakdown. Raggedy clumps of jet-black hair fell across Hamdi’s thick-rimmed glasses. His last haphazard shave three days ago and his hooded, droopy eyes made him appear like he was permanently ensconced in a shadow. Hamdi’s white coat was misbuttoned and the left side hung six inches lower than the right. His stethoscope was dangling out of the left pocket, scraping the floor as he walked. Hamdi never wore anything but scrubs, usually mismatched blues and greens.
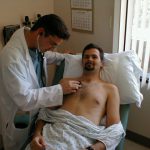 Hamdi was the type of intern who was petrified at the prospect of being caught unprepared, and thus lugged every possible portable medical paraphernalia, book, card, and cheat sheet with him to shield against the infinite number of challenges lurking in the wards. Despite the fact every nurses’ station on every floor was adequately equipped with supplies for IVs and blood draws, Hamdi’s pockets were crammed with blood tubes (red-tops, blue-tops, speckle-tops, purple-tops), alcohol swabs, iodine swabs, gauze pads (2x2s and 4x4s), tourniquets, IVs (22 gauge, 20 gauge, 18 gauge, 16 gauge, and even 14 gauge in case he happened upon someone who was exsanguinating and needed an IV the diameter of a Bic pen). Two needle-nose clamps were clipped onto the top two button-holes of his coat, sporting rolls of cloth tape and paper tape. The third buttonhole was home to a rubber-nosed reflex hammer. The other pockets bulged with EKG attachments, sputum cups, index cards, laminated cards of medical protocols, pocket books of formulas, rulers, calipers, stampers, and spare beeper batteries. However, three pockets-worth of medical paraphernalia were not enough to assuage his existential intern angst, and so Hamdi also carried in his hands an overstuffed, drug-company-dispensed clipboard advertising the second-costliest ulcer medication, an assiduously dog-eared copy of the Washington Manual of Medical Therapeutics, a hot-pink three-ring binder (touting the latest broad-spectrum antibiotic) from which papers were spilling out at every angle, last-year’s hospital phonebook, and the takeout menu from Chi-Chi’s—the local Mexican fast food joint run by Koreans who’d developed an impressively efficient way of turning out the dirt-cheap, passably edible chicken fajitas that were Hamdi’s daily salvation from the unrelenting intern paranoia that he was just nanoseconds from inadvertently killing, maiming, or otherwise harming one of his patients.
Hamdi was the type of intern who was petrified at the prospect of being caught unprepared, and thus lugged every possible portable medical paraphernalia, book, card, and cheat sheet with him to shield against the infinite number of challenges lurking in the wards. Despite the fact every nurses’ station on every floor was adequately equipped with supplies for IVs and blood draws, Hamdi’s pockets were crammed with blood tubes (red-tops, blue-tops, speckle-tops, purple-tops), alcohol swabs, iodine swabs, gauze pads (2x2s and 4x4s), tourniquets, IVs (22 gauge, 20 gauge, 18 gauge, 16 gauge, and even 14 gauge in case he happened upon someone who was exsanguinating and needed an IV the diameter of a Bic pen). Two needle-nose clamps were clipped onto the top two button-holes of his coat, sporting rolls of cloth tape and paper tape. The third buttonhole was home to a rubber-nosed reflex hammer. The other pockets bulged with EKG attachments, sputum cups, index cards, laminated cards of medical protocols, pocket books of formulas, rulers, calipers, stampers, and spare beeper batteries. However, three pockets-worth of medical paraphernalia were not enough to assuage his existential intern angst, and so Hamdi also carried in his hands an overstuffed, drug-company-dispensed clipboard advertising the second-costliest ulcer medication, an assiduously dog-eared copy of the Washington Manual of Medical Therapeutics, a hot-pink three-ring binder (touting the latest broad-spectrum antibiotic) from which papers were spilling out at every angle, last-year’s hospital phonebook, and the takeout menu from Chi-Chi’s—the local Mexican fast food joint run by Koreans who’d developed an impressively efficient way of turning out the dirt-cheap, passably edible chicken fajitas that were Hamdi’s daily salvation from the unrelenting intern paranoia that he was just nanoseconds from inadvertently killing, maiming, or otherwise harming one of his patients.
“What’s up, Hamdi?” Graham asked, seeing in Hamdi a little bit of himself when he was an intern.
Hamdi shook his head heavily, panting, and the metal clamps and reflex hammer hanging from his coat jangled. It took him a minute to catch his breath. “Yalena told me to go see the skin-popper, but I’ve been with the fever guy for an hour trying to get an IV in.” Hamdi’s face tautened as he said this, as though this were just the latest in a long day of death and destruction.
“Not to worry,” Graham said, suppressing a desire to pat Hamdi on the head like a wayward puppy. “I already saw Milford, already paged plastics. Why don’t you run along and take care of all the rectals on 16-West?”
Hamdi pursed his lips grimly. “Nope, Yalena’s already paged me. Got to review all the admissions with her.” He consulted his scut list, then marched away. The slight limp of his right leg could sometimes be masked when Hamdi was calm and focused. But when he was stressed and overwhelmed—as he was now, and indeed most of his waking hours—the limp was more pronounced. His left leg took on the business of ambulating forward, and his right leg swung around like the free arm of a compass. This lent a rhythmic cadence to his stride, an accented downbeat followed by a more measured reply. After four of these syncopated couplets, Hamdi plunged into the ER cacophony, head bent down as though there would be no passage unless he rammed his way though.
Graham jammed his hands in his pants pockets and then followed Hamdi back to the procedure room, where the team was conferring over the list of admissions with Yalena. Yalena was a reasonably competent second-year resident, with a placid demeanor that only partly obscured an iron resolve to get ahead. Selections for chief residents were made toward the middle of the second year of residency, and Yalena—though she wouldn’t say it aloud—was determined to be one of that select group of four.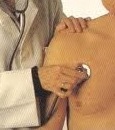
Yalena’s face was a pale orb with little in the way of contrasting features. Her eyes, lashes, and lips were nearly the identical color as the rest of her skin. That and the complete absence of wrinkles, freckles, smudges, scars, birthmarks or moles gave her face an egg-like smoothness that seemed almost unnatural. Her perfectly straight brown hair was always pulled back from her face in a tight ponytail. A wide black elastic headband was positioned exactly at the hairline at the edge of her forehead, so that her hair didn’t seem to “appear” until several inches back on her head. This added another element of odd featurelessness to her milky visage.
Yalena’s head was always slightly cocked upward, as though she were trying to see upward over the horizon. When she walked, this gave the impression that she was leading with her nose. Her pale, close-lipped smile straddled the border of angelic and condescending, but her attitude on a call day—which Graham respected and appreciated—was all-business.
“Okay,” she said, tapping her list with her trademark fountain pen, “there’s a chest pain, an altered mental status, a lupus flare, and a diarrhea guy. Rumor has it that there’s a GI bleeder in the works. I’ll send the medical students to check out the lupus case. Hamdi, you eyeball the diarrhea guy and make sure he’s stable. I’ll check on the altered mental status lady and see whether she needs a spinal tap. Dr. Brenfield, do you mind seeing the chest pain guy?”
Graham nodded his head. He much preferred sharing the workload upfront with the team. He could skip the niceties of academic discussions and touchy-feely connections. Basically, there were X number of admissions to which he’d have to sign his name as the legally responsible physician, and he’d just as well get them over with as soon as possible.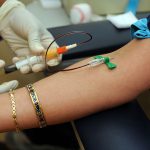
“Oh, and the guy from this morning with the possible pulmonary embolus…,” Yalena called out to Graham as he began to walk away, “his lung scan came back as “indeterminate.” I kept him on heparin anyway, just in case.”
“You think he really has a blood clot” Graham asked, turning back to Yalena.
Yalena shrugged. “Maybe. But better safe than sorry. I figured we’d leave on him the blood thinner for now, until we work up other possibilities.”
“But there are side effects to heparin,” Graham said, feeling himself shift into educational mode. “He could bleed.”
“Not if we monitor it correctly,” Yalena replied, snapping her fountain pen closed and sliding it neatly into her pocket.
“A hundred thousand people die every year in this country from adverse medication reactions,” Graham said, looking from Yalena to Hamdi. “One hundred thousand. We kill patients all the time with our treatments. Just keep that in mind, guys, as you go about your business. Everything we do in medicine has the potential to do harm.” Hamdi looked faint.
Graham and his team plowed through their roster of admissions for the day. By 10 pm, most of the patients were “tucked in,” as the expression went. The obese 76 year-old Puerto Rican man with crushing chest pain was in the CCU after the cardiologists stented open his clogged right coronary artery. The obtunded 91-year-old, transferred from a nursing-home with “altered mental status” had been found to have a urinary tract infection, and broad-spectrum antibiotics were already flowing through her spindly veins. The winsome, 24 year-old Honduran woman with a flare of lupus nephritis was leafing through Vanidades fashion magazine and chatting on her cell phone while the nurses set up her cyclo-phosphamide treatment. The 36 year-old white gay man with profuse AIDS-related diarrhea was still pouring out diarrhea, but was actually feeling better, thanks to the aggressive IV hydration. The 53 year-old guy with the possible blood clot turned out to have a pneumonia and was now getting antibiotics instead of blood thinners. The 64 year-old alcoholic with bleeding duodenal ulcers had just been scoped by the GI fellow, when a code was called down the hall from where Graham was sitting, writing an admission note, in the 16-North nurses’ station.
Usually, Graham let the residents handle the codes—the residents being far nimbler in their recollection of ACLS protocols—but being so nearby he felt obliged to at least check it out until the rest of the team navigated East Memorial’s unreliable elevators to get to the sixteenth floor. “In the bathroom,” one of the nurses shouted to him, pointing the way. Graham barreled his way in, and there on the gray tile floor was Cherry Milford, crumpled under the sink, a syringe still poking out of her cavernous thigh ulcer. A respiratory technician was hunched near the commode, trying to stabilize Milford’s airway. “I can’t do it here,” he grunted. “Help me get her out.”
Graham and the technician dragged Milford’s slack body out of the bathroom and heaped her onto a bed. “Shot up in that disgustingly infected ulcer,” the technician said, strapping the oxygen mask over the patient’s mouth as the code team arrived and sprang into action. “Pathetic.”
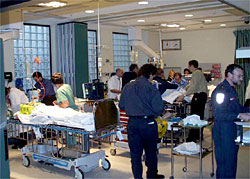 The full code proceeded—chest compressions, electric shocks, breathing tube, central lines, blood gases, ampules of epinephrine, atropine, Narcan, bicarb—but it was clear that Cherry Milford was dead. She’d managed to OD in the bathroom of East Memorial just as she would have done in the hallway of the crack house or an unused subway entrance. The only difference was that she had been discovered by a nurse and so her corpse was subjected to a host of “life-saving” procedures. From the first time the Paris Academy of Sciences recommended, in 1740, that mouth-to-mouth resuscitation be administered to drowning victims, resuscitation protocols had been elaborated specifically for otherwise-healthy patients who experienced an acute insult to their well-being. The current Advanced Cardiac Life Saving algorithms on display at this moment had been developed for the cardiac patient who experienced a sudden arrhythmia that could be shocked back into normalcy. They had not been developed with the likes of Cherry Milford in mind.
The full code proceeded—chest compressions, electric shocks, breathing tube, central lines, blood gases, ampules of epinephrine, atropine, Narcan, bicarb—but it was clear that Cherry Milford was dead. She’d managed to OD in the bathroom of East Memorial just as she would have done in the hallway of the crack house or an unused subway entrance. The only difference was that she had been discovered by a nurse and so her corpse was subjected to a host of “life-saving” procedures. From the first time the Paris Academy of Sciences recommended, in 1740, that mouth-to-mouth resuscitation be administered to drowning victims, resuscitation protocols had been elaborated specifically for otherwise-healthy patients who experienced an acute insult to their well-being. The current Advanced Cardiac Life Saving algorithms on display at this moment had been developed for the cardiac patient who experienced a sudden arrhythmia that could be shocked back into normalcy. They had not been developed with the likes of Cherry Milford in mind.
“Suicide,” the technician commented to Graham, who stood at his side watching the oxygen being forced into the breathing tube. “Self-inflicted death by needle. Pathetic.”
It was pathetic, Graham thought. It was pathetic that a leg nearly eaten away to the bone was not a deterrent to snarfing up more drugs; it was merely a vehicle. It was pathetic that Cherry Milford’s body was so sapped of biological reserve that the thousands of dollars of equipment and medications being used in this code could never revive it. It was pathetic that the scaffolding of society was so porous that entire lives could slip through and self-destruct. It was pathetic that Graham’s dead patient was exactly the same age as he was. And what was most pathetic of all, was that despite all of these swirling thoughts in his head, what Graham was most agitated about was that he still had one more admission note to write before he could get out of the hospital.
(excerpt from unpublished novel, “Malignancy.” Originally appeared in “2 Bridges Review” pg 86)
