Incidental Finding?
by Danielle Ofri
New York Times
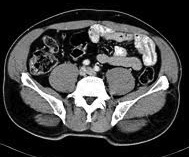
An incidental finding — I was convinced of it. My patient had undergone a CT scan of the abdomen at another hospital because of stomach pains and “incidentally noted” was a 2-centimeter mass in her adrenal gland. She brought in the report for me to see, nervous that she might have cancer.
I reassured her that it was exceedingly unlikely that she had cancer. Benign masses in the adrenal gland are nearly as common as birthmarks. They almost never cause symptoms and we stumble across them only because we do so many scans for other reasons. They’ve even earned their own appellation: incidentalomas, and that’s what I was sure she had.
Of course a tiny fraction — 1 to 2 percent — of these adrenal masses can wreak havoc by churning out an excess of adrenal hormones or by being cancerous. Luckily, the mass on my patient’s scan possessed all the reassuring characteristics of benignity: it was small, low-attenuating, well circumscribed, with smooth borders. And she had no symptoms to suggest adrenal hyperactivity or cancer. It was most likely a benign adrenal adenoma that would never cause her harm.
Nevertheless, once the incidentaloma had been given life, so to speak, it was no longer incidental. We were now obliged to run some highly complicated – and expensive – lab tests. I winced as I ordered urinary metanephrines to test the adrenaline-producing capacity of the adrenal. The computer warned me with exclamation points and asterisks that this was a “greater-than-$100-send-out test.” Explaining how to correctly collect a 24-hour urine sample was its own involved discussion. Then I had to explain the even more complicated logistics of the overnight dexamethasone-suppression test to evaluate the cortisol-producing capacity of the adrenal.
After that, I considered the follow-up CT scans, recommended at six months, one year and two years, to ensure that the mass wasn’t growing. What about all that radiation? One group of endocrinologists estimated that the chance of uncovering a malignant cancer in patients like mine was roughly equal to the chance of causing a fatal cancer from the radiation of these follow-up CT scans. And might these CT scans pick up other incidental findings, opening yet more Pandora’s boxes of medical evaluation?
And what about the issue of skyrocketing medical costs? The evaluation of this incidentaloma was going to cost more than a thousand dollars. Tens of millions of CT scans are done every year in the United States. It doesn’t take many back-of-the-envelope calculations to see how quickly the costs of incidental findings, and their subsequent evaluations, add up. How much should the societal obligation weigh into the decisions for my patient?
My thoughts flitted back to the doctor who had ordered this CT in the first place. Perhaps if the doctor had had more time to spend on the history and physical, the CT would not have been necessary. From my 15 years with this patient, I knew that her symptoms could be voluminous in quantity and quality. This wasn’t to say that something serious couldn’t squeak in, but over the years I have learned that it takes immense perseverance and patience to tease out the significance of each symptom. Otherwise we’d be doing a CT every week for her.
But I could understand how a doctor in a busy ER on a weekend might have been overwhelmed by the plethora of symptoms and simply ordered a CT “to be on the safe side.” I wished that doctor had tried to call me before ordering the scan, but what’s done was done. The fallout of that decision was now in my lap.
By now we had run well over our allotted time and my patient was utterly overwhelmed by the complex testing procedures and schedules. The adrenal mass was an incidental finding, after all, but it had completely steamrolled our visit. My patient’s diabetes, obesity, depression, arthritis and elevated cholesterol all ended up with the short end of the clinical stick – an outcome that surely is not incidental to her health. (from the New York Times)